Community Corner highlights the work of Seattle Human Services’ community partners in their own words. Our goal is to gather stories and photos that illustrate their amazing work on behalf of the people of Seattle. This post focuses on the Opioid Recovery & Care Access (ORCA) Center, a facility operated by the Downtown Emergency Service Center (DESC) that provides care and resources for individuals facing opioid use disorder.
The Human Services Department has funded the development and growth of DESC’s innovative ORCA Program since its inception, including directing nearly $1 million in opioid settlement funds and leveraging Community Development Block Grant funds to open the ORCA Center in the summer of 2025. In 2026, more than $3 million in additional funding made possible by the Mayor’s Office and Seattle City Council has gone toward ORCA Center operations and expanding a mobile service model called ORCA POD.
In this blog post, Jessica Schreindl, DESC senior communications manager, provides details about how the ORCA Center’s “no wrong door” approach is tackling both the immediate crisis of overdose and the long-term needs of recovery and stability. Visit the ORCA Center webpage and follow DESC on Facebook, Instagram and LinkedIn.

What is the ORCA Center and what is the ORCA POD?
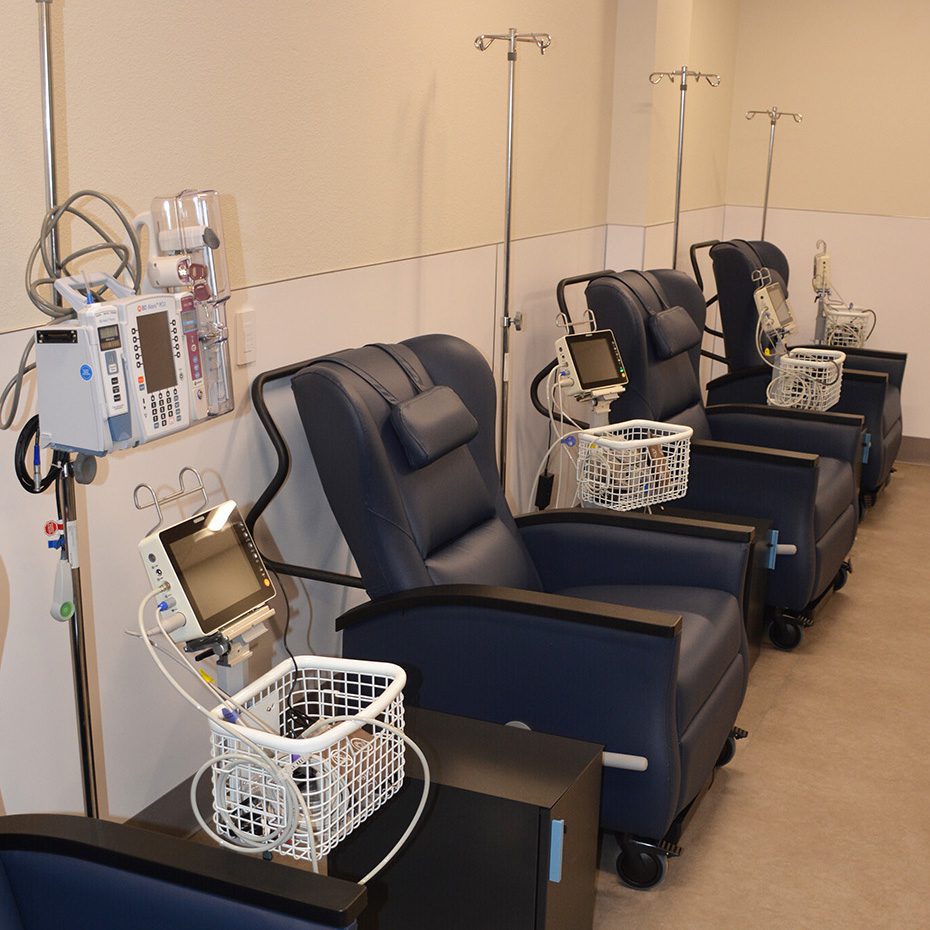
The Opioid Recovery & Care Access (ORCA) Center is a 24/7, low-barrier facility operated by DESC that provides immediate, compassionate care for people after an opioid overdose, along with same-day access to medication for opioid use disorder (MOUD). Located within DESC’s Downtown Behavioral Health Clinic, it offers a safe, judgment-free space where people can stabilize, begin treatment, and connect to ongoing care and services.
The ORCA Patient Outreach Division (POD) extends this care into the community — bringing treatment directly to people in DESC permanent supportive housing and shelters.
The program was created in response to the dramatic rise in opioid overdoses and deaths — particularly driven by fentanyl — and longstanding gaps in access to treatment. Many people were cycling through hospital emergency rooms without getting connected to ongoing care, and only a fraction of those who needed treatment were receiving it. ORCA was designed to fill that gap by offering rapid, accessible care and clear, evidence-based pathways to recovery.
What is medication for opioid use disorder (MOUD), and how does it help people with opioid use disorder?
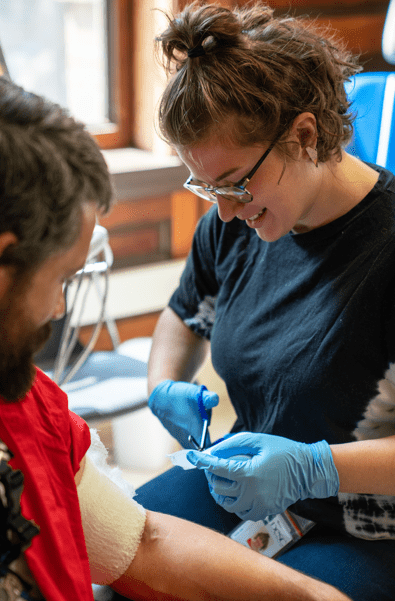
The term medications for opioid use disorder (MOUD) refers to FDA-approved medications — such as buprenorphine and methadone — that help treat opioid addiction. These medications work by reducing cravings and withdrawal symptoms, stabilizing brain chemistry, and lowering the risk of overdose.
At a high level, MOUD allows people to move out of the cycle of withdrawal and use, creating the stability needed to focus on their health, housing, and long-term recovery. It is considered the gold standard of care for opioid use disorder and has been shown to significantly reduce overdose deaths and improve outcomes.
What is new or innovative about the work of the ORCA Center and ORCA POD?
ORCA represents a fundamentally different approach to opioid treatment — centered on immediacy, accessibility, and meeting people where they are.
Key innovations include:
- 24/7 post-overdose stabilization outside of hospital settings, reducing reliance on emergency rooms.
- Same-day access to MOUD with extended walk-in hours from 9 a.m. to 11 p.m. every day, year-round — eliminating delays that often prevent people from starting treatment.
- Access to long-acting injectable buprenorphine, a highly effective medication administered as a monthly injection, eliminating the need for daily doses.
- Low-barrier, voluntary care, with no requirement to engage in treatment to receive support.
- Integration with behavioral health, housing, and outreach services, creating a “no wrong door” approach.
- Mobile, community-based care through ORCA POD, which brings MOUD directly to clients rather than requiring them to come to a clinic.
Together, these elements create a more humane and effective model that addresses both the immediate crisis of overdose and the long-term needs of recovery and stability.
How do people remain connected to services after their initial intake? What are the next steps?
Care at the ORCA Center is designed to extend well beyond the initial visit. From the moment someone arrives, discharge planning begins — connecting individuals to ongoing treatment as well as long-term supports like behavioral health care and housing resources.
Clients can continue receiving MOUD through follow-up care at the ORCA Center or through referrals to other community providers. The ORCA POD team plays a critical role in maintaining engagement by delivering care directly to clients where they live and helping ensure continuity of treatment — especially for those who may face barriers to accessing clinic-based care.
What’s something the community might not know about the ORCA Center or the clients you serve?
One thing many people may not realize is that most individuals accessing the ORCA Center are actively walking in for ongoing treatment, rather than for post-overdose care. In fact, the majority of visits are for medication for opioid use disorder (MOUD), not emergency stabilization.
Another important point is that ORCA serves people with highly complex needs, including homelessness, serious mental illness, and chronic health conditions. Recovery is not a single moment — it’s a process that requires consistent support, trust-building, and access to multiple services. ORCA is designed to meet people at whatever point they are in that journey, without judgment or preconditions.
What early successes or outcomes have occurred since the ORCA Center opened?
Early outcomes show strong engagement and impact from the ORCA Center and POD teams:
- 5,700 encounters in the first seven months, including both post-overdose care and walk-in treatment.
- More than 1,100 clients served in that same period.
- 540 people started on MOUD — including high adoption rates of long-acting injectable buprenorphine — while hundreds more already on MOUD continued to receive ongoing treatment and support._
Additionally, early data shows that the ORCA program is successfully connecting people to longer-term care, housing resources, and recovery supports — helping reduce strain on emergency departments and first responders.
DESC’s ORCA Center is located at 515 3rd Ave. in downtown Seattle. To gain admission after hours (11 p.m. to 9 a.m.) use the buzzer at the door to the right.